The Complete, Central-Enhanced Guide
Screening patients for glaucoma or neuro-ophthalmic disease still begins with the 24-2 visual field exam, but today’s clinicians also rely on the newer 24-2C visual field pattern for even more sensitivity in the central retina. This guide demystifies both tests and shows how head-mounted perimeter solutions such as Virtual Field deliver a more comfortable, accurate, and billable glaucoma progression test.
What is the 24-2 Visual Field Exam?
The 24-2 visual field test divides the central 24° into 54 threshold points. A light stimulus dims or brightens until the patient detects it, mapping retinal sensitivity across the near-periphery.
- Primary use: Early-stage glaucoma progression test
- Secondary uses: Optic neuropathies, stroke, brain lesions, diabetic or hypertensive retinopathy, macular degeneration
It’s best known as a glaucoma detection test that reliably identifies patterns such as nasal steps and arcuate scotomas, but it can also diagnose and monitor many other conditions.
Occasionally, you’ll see the 24-2 test called the HVF 24-2 or the Humphrey visual field exam. This name is a reference to the Humphrey visual field perimeter, which has been historically used to conduct this test since the 1980s. However, using a Humphrey Visual Field Analyzer to conduct this exam is not strictly necessary. Carrot is an innovative, streamlined, and patient-friendly alternative.
Key upgrade: Using a portable threshold perimeter such as the Carrot headset slashes setup time, reduces patient fatigue, and produces “functionally indistinguishable” results compared with the Humphrey Field Analyzer (HFA).
Academic references and clinical validation
|
|
The Full Field 120 is a suprathreshold exam, and this study showed that exams of this type perform well to screen for glaucoma. |
|
|
Research by Hood et al. (2022) compared the diagnostic accuracy of 24-2 and 10-2 perimetry tests. They found that the 24-2 test had better overall diagnostic accuracy, with a higher area under the ROC curve (0.808) compared to the 10-2 test (0.742). Results support the validity of the 24-2 exam by demonstrating its superior diagnostic accuracy compared to another commonly used test, reinforcing its effectiveness in clinical practice. |
|
|
Recent research by Kahook and Noecker highlighted the importance of proper interpretation of the 24-2 Humphrey Visual Field printout, emphasizing factors such as pupil diameter and appropriate refraction that can influence test outcomes. |
The 24-2 exam is the most common visual field test Carrot performs. In fact, Carrot users around the world conduct one of these exams every 12 seconds.

Clinical Validation of Carrot’s 24-2 exam
|
Another study compared virtual reality visual field testing to Humphrey visual field testing in an academic ophthalmology practice. The results showed that virtual visual field testing had similar accuracy to Humphrey virtual field testing but offered additional advantages like shorter test duration, fewer false positives, and lower costs. |
In 2024, Carrot (formerly Virtual Field) received the Medical Device Single Audit Program (MDSAP) certification, verifying that our leading eye exam experience meets rigorous international standards, including ISO 13485:2016 and the stringent U.S. Food and Drug Administration (FDA) requirements. |
One study compared the Carrot (formerly Virtual Field) head-mounted perimeter to the Humphrey Field Analyzer in glaucoma and optic nerve disease patients. Researchers described the output as “functionally indistinguishable” to the Humphrey Visual Field Analyzer. |
24-2 at a Glance — Pros, Cons, and Workflows
Ophthalmologists appreciate the 24-2 visual field exam for its ability to detect subtle, early visual field defects and monitor progression in conditions such as glaucoma and optic neuropathies, providing reliable, repeatable results that are crucial for managing chronic diseases.
However, they often express frustration with the test’s limitations on traditional tabletop devices, such as the lengthy, fatiguing process, reliance on patient cooperation, and the need for expert interpretation of complex reports. Thankfully, Carrot addresses some pain points by improving patient comfort and streamlining workflows. For example, our DICOM 360 Sync transforms exam workflows into a fully connected, zero-touch experience — from patient setup to report sync to record attachment.
Workflow tip: The Carrot head-mounted perimeter also lets techs test either eye in under three minutes, freeing the exam lane for refractions or imaging.
Pros and cons of the 24-2 exam
|
Pros
|
Cons
|
Diseases and Disorders Detected With 24-2
|
|
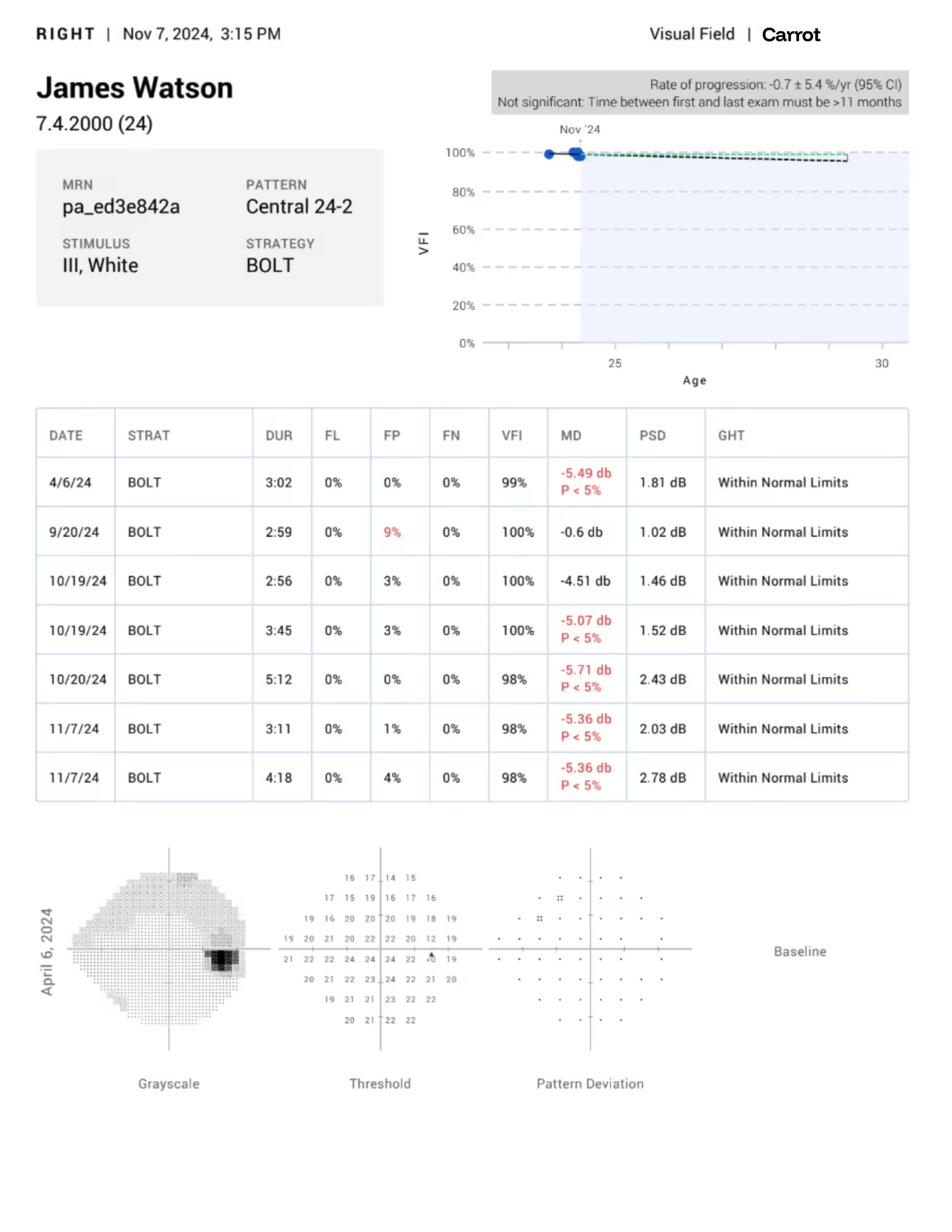
Example 24-2 Reports
1 / 7
24-2C: Central-Enhanced Visual Field Testing
Introduced in 2019, the 24-2C visual field pattern adds 10 central points inside the 10° region—capturing early macular damage without the time penalty of running both 24-2 and 10-2.
Like its predecessor, the 24-2C divides the central 24 degrees of a patient’s vision into a grid to identify changes in the visual field. The 24-2C test includes the 54 points from the standard 24-2 test, plus 10 additional test points within the central 10 degrees of vision. The “C” refers to increased sensitivity in detecting central vision defects, which can indicate glaucoma progression.
Before the introduction of this test, data with this level of detail required administering both the 24-2 and the 10-2 exam. Combining the two saves time for both your workflow and your patients.
Academic references and clinical validation
|
|
The introduction of the 24-2C visual field test compares the 24-2 and 10-2 testing patterns, which traditionally were completed separately. Initial research shows that the 24-2C is comprehensive and can be treated as a hybrid test. |
|
|
Another study compared the performance of the 24-2C and 10-2 test grids in patients with glaucoma and people suspected of having the condition. Both grids produced similar overall results, but the 10-2 detected more central visual field defects and showed better alignment with OCT scans. The 24-2C was faster, whereas the 10-2 provided more detailed insights. |
|
|
One study evaluated the effectiveness of 24-2C, 24-2, and 10-2 visual field tests for detecting mild-stage glaucoma with central visual field defects. The 24-2C demonstrated superior detection accuracy, particularly in the upper-central visual field. It also significantly reduced test duration when compared to 24-2 and 10-2. |
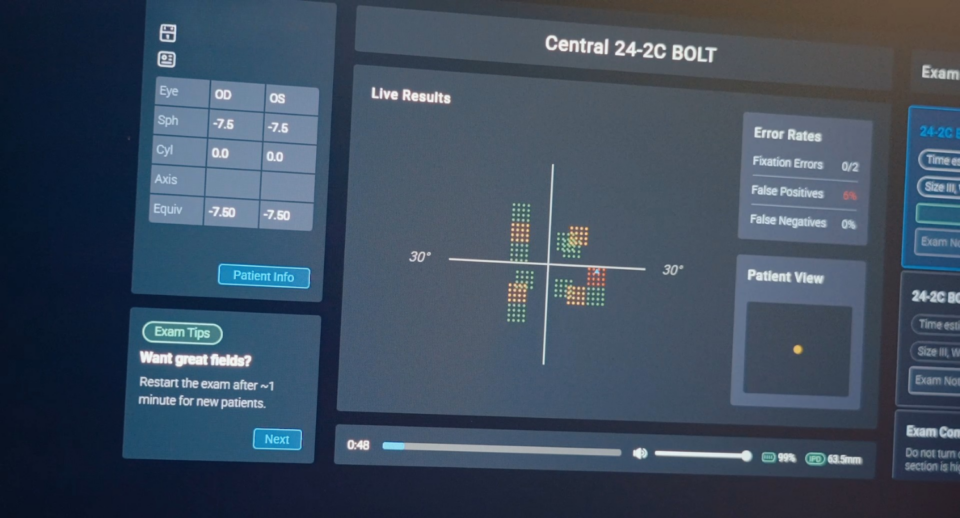
Conducting the 24-2C with Carrot
In 2024, Carrot (formerly Virtual Field) added the 24-2C to our suite of visual field exams. This testing capability was automatically added to all Carrot subscriptions, so there’s no extra cost or need to upgrade. Simply update your software to the latest version to begin offering the 24-2C.
Whether you choose the traditional 24-2 or newer 24-2C, the testing and billing processes are the same.
Billing and Coding (CPT 92083)
The 24-2 visual field exam is billable to insurance under CPT code 92083, which is designated for extended visual field exams.
- CPT 92083 – Extended visual field examination
- Typical Medicare Physician Fee Schedule (MPFS) reimbursement: $40–$90 (U.S.). Exact fees will, of course, depend on your location, setting, and payer-specific factors.
- Cadence:
- Early glaucoma: Every 6–12 months
- Moderate–advanced: Every 3–6 months
- Systemic risk (DM, HTN, meds): As clinically indicated
When is the 24-2 exam required?
The 24-2 is a standard baseline exam for glaucoma patients. You can expect to re-examine people with early-stage glaucoma every six months to a year. For moderate to advanced glaucoma, cadence increases to every three to six months to monitor disease progression.
People often don’t notice changes to their visual field, so this exam is also ordered for patients with diabetes, hypertension, or a family history of eye disease. People taking certain medications known to increase intraocular pressure may also need the 24-2 exam to monitor visual changes.
Is the 24-2 visual field test required for driver’s licenses?
The 24-2 exam is more advanced than the basic field-of-vision checks required for driver’s licensing. Currently, this exam isn’t specifically mandated for drivers in the United States or Canada.
However, many states require a horizontal visual field of 120 degrees or better. In Canada, provinces have standards for visual acuity and peripheral vision, but don’t specify the 24-2 test. That said, if you incorporate the 24-2 into your routine exams, the detailed results can support the information necessary for driver’s licensing.
Start Conducting the 24-2 and 24-2C Exams with Carrot
The 24-2 visual field report is a wealth of diagnostic information when interpreted correctly. Diagnose, monitor, and manage a wide range of ocular and neurological conditions, ranging from glaucoma to brain tumors.
Want all 23 of our comprehensive test guides in your inbox? Fill out the form below.
Frequently Asked Questions
24-2C adds 10 extra central test points atop the standard 54, boosting sensitivity to early macular glaucoma without increasing test time by more than 30 seconds per eye.
No. Both fall under CPT 92083; insurers do not differentiate patterns.
Most specialists schedule every six months; fast progressors (≥ 1 dB/yr MD loss) merit quarterly testing.
Yes. With Carrot, you can switch patterns in the dashboard without recalibration. The headset auto-loads age-adjusted normative data for each.
No. The bright background (10 cd/m²) is designed for pupils as small as 2 mm. Dilation is unnecessary.
The software plots MD, PSD, and Visual Field Index (VFI) regression and highlights P < 0.05 slopes for easy chart review.
24-2C inserts ten strategically placed points inside the macular region (<10°) that correspond to the retinal nerve fiber bundle most often damaged first in glaucoma; a recent AAO study showed 24-2C detects progression 15% earlier than 24-2 alone.
Yes. Cataract surgery can affect the mean deviation (MD) results of 24-2 and 24-2C visual field tests. Immediately after clear-cornea phaco, MD typically improves 1–2 dB because forward light scatter is removed; document lens status so postoperative MD gains don’t mask true glaucoma progression.
Carrot offers a “Rapid Recheck” mode that masks previously seen stimuli and repeats only the flagged points. This confirmation run takes under 60 seconds per eye and solidifies true positives before you close the chart.
Keep fixation losses <20%, false-positives <15%, and false-negatives <15%. The headset’s eye-tracking reticle minimizes fixation loss, but high false-positive rates (>15%) often mean patient trigger-happy responses. Schedule a repeat test if these data points are exceeded.