The Importance of Visual Field Testing in Glaucoma Care
Automated visual field testing is an essential tool in diagnosing and monitoring glaucoma. Clinicians rely on perimetry to detect functional vision loss, identify scotomas, and monitor disease progression over time.
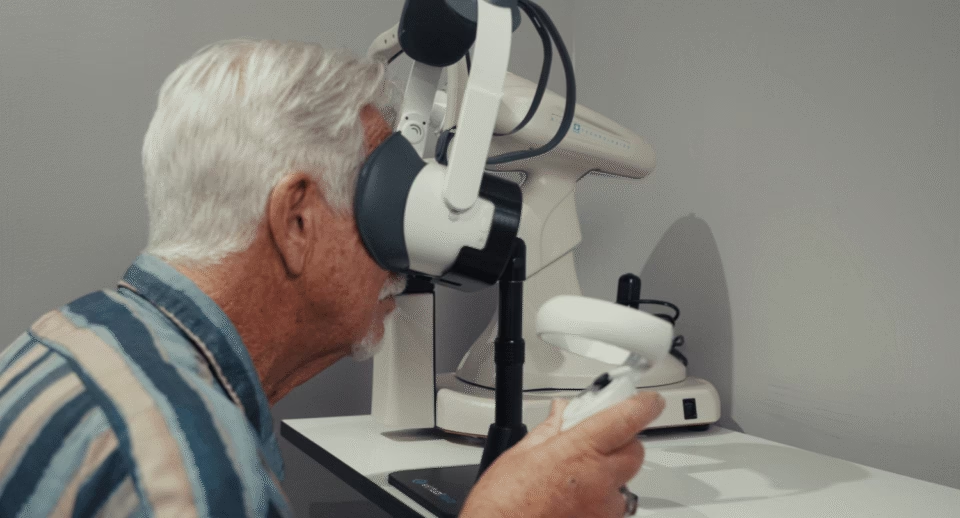
The Humphrey Field Analyzer using the 24-2 SITA Standard protocol remains one of the most widely used systems for automated perimetry in clinical practice.
However, traditional visual field machines are large, expensive, and require dedicated testing space, which can limit access to testing and constrain clinic workflow.
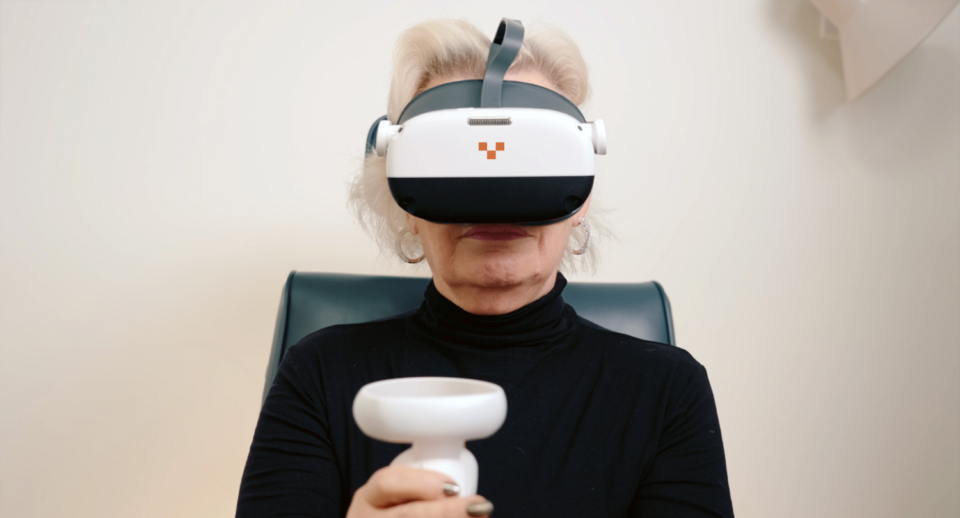
Virtual reality visual field testing provides an alternative approach by using head-mounted VR technology to perform visual field assessments in a portable format.
“Virtual reality perimetry may expand access to visual field testing while maintaining clinically meaningful accuracy.”
Study Overview
This study evaluated how results from the Virtual Field VR visual field platform (now Carrot) compare with the Zeiss Humphrey 24-2 SITA Standard test in patients with known glaucoma-related visual field defects.
Researchers focused on patients with established glaucoma and known scotomas who were returning for routine visual field testing in a comprehensive ophthalmology practice.
The goal was to determine whether VR-based testing could produce results comparable to the clinical standard while offering practical advantages for clinics.
Study Population
The study included 50 eyes from 31 patients undergoing routine glaucoma monitoring.
All participants had established glaucoma with previously documented visual field defects.
Each patient completed two visual field tests during the same visit:
- Humphrey-Zeiss 24-2 SITA Standard visual field test
- Virtual reality visual field test using the Virtual Field platform (now Carrot)
The VR test was performed within five minutes of completing the Humphrey test, allowing researchers to directly compare results under similar testing conditions.
Testing Method
After completing the Humphrey visual field test, patients immediately performed the VR-based visual field test.
Researchers then analyzed the results from both tests to evaluate similarities and differences across several key clinical metrics, including:
- Visual Field Index (VFI)
- Mean Deviation (MD)
- Pattern Deviation (PD)
Statistical analysis included Pearson correlation coefficients and intraclass correlation coefficients to evaluate agreement between the two testing methods.
Clinical Results
Overall, the study demonstrated strong correlations between VR visual field testing and the Humphrey standard.
Visual Field Index
Virtual Field showed excellent correlation with Humphrey measurements for the visual field index.
- Pearson correlation: 0.93 (p < 0.00001)
- Intraclass correlation: 0.99
Although the VR system produced slightly lower VFI values on average, the measurements remained highly correlated between devices.
Mean Deviation
Mean deviation also showed a strong correlation between the two systems.
- Mean difference: -3.03 dB
- Pearson correlation: 0.85 (p < 0.00001)
- Intraclass correlation: 0.74
Pattern Deviation
No significant differences were observed between the two devices for pattern deviation, which measures localized visual field defects.
- Pearson correlation: 0.79 (p < 0.00001)
- Intraclass correlation: 0.81
These findings indicate that VR-based visual field testing can produce clinically meaningful measurements comparable to the Humphrey standard.
Practical Advantages of VR Visual Field Testing
In addition to strong clinical agreement with traditional testing, virtual reality perimetry offers several practical benefits for ophthalmology practices.
Because VR testing uses a portable headset rather than a large perimeter device, it can be deployed in a wider range of clinical settings.
Potential advantages include:
- Improved mobility, allowing testing outside specialized visual field rooms
- Lower equipment costs compared to traditional perimetry machines
- Improved clinic efficiency through flexible testing workflows
- Expanded access to visual field testing
These benefits may be particularly valuable for clinics seeking to increase testing capacity or reduce infrastructure requirements.
“Virtual Field shows promise in increasing mobility, efficiency, and cost reduction while maintaining testing accuracy.”
Future Directions
While the results are encouraging, additional research will continue to explore how VR visual field testing performs across larger patient populations and over longer monitoring periods.
Future research may focus on:
- Longitudinal glaucoma progression monitoring
- Test-retest reliability of VR measurements
- Integration of VR testing into routine clinical workflows
As virtual reality technology continues to evolve, it may play an increasingly important role in modernizing visual field testing and expanding access to glaucoma care.
Study Citation
Comparison of a Virtual Reality Visual Field Program to the Zeiss Humphrey 24-2 SITA Standard in a Comprehensive Ophthalmology Practice.
Presented at the American Society of Cataract and Refractive Surgery (ASCRS) Annual Meeting.